Man 'cured' of HIV following discovery of brother's rare genetic mutation
Only a handful of patients have ever seen their human immunodeficiency virus go into long-term remission

There's been a medical breakthrough as a man from Oslo has been functionally 'cured' of HIV following a stem cell transplant from his brother.
Although human immunodeficiency virus can currently be controlled by medication, it tends to rebound when treatment is stopped. This makes the case of the 63-year-old man simply known as 'the Oslo patient' something of a big deal on the science scene.
The main issue with HIV is that it can remain hidden in pockets of cells, although health studies suggest that stem cell transplants from healthy donors can put the body into remission. It's thought that those with a specific genetic mutation of CCR5Δ32/Δ32 have the ability to remove the receptor proteins that HIV needs to infect cells.
Diagnosed with HIV at the age of 44 in 2006, the patient then developed a rare type of blood cancer.
Advert

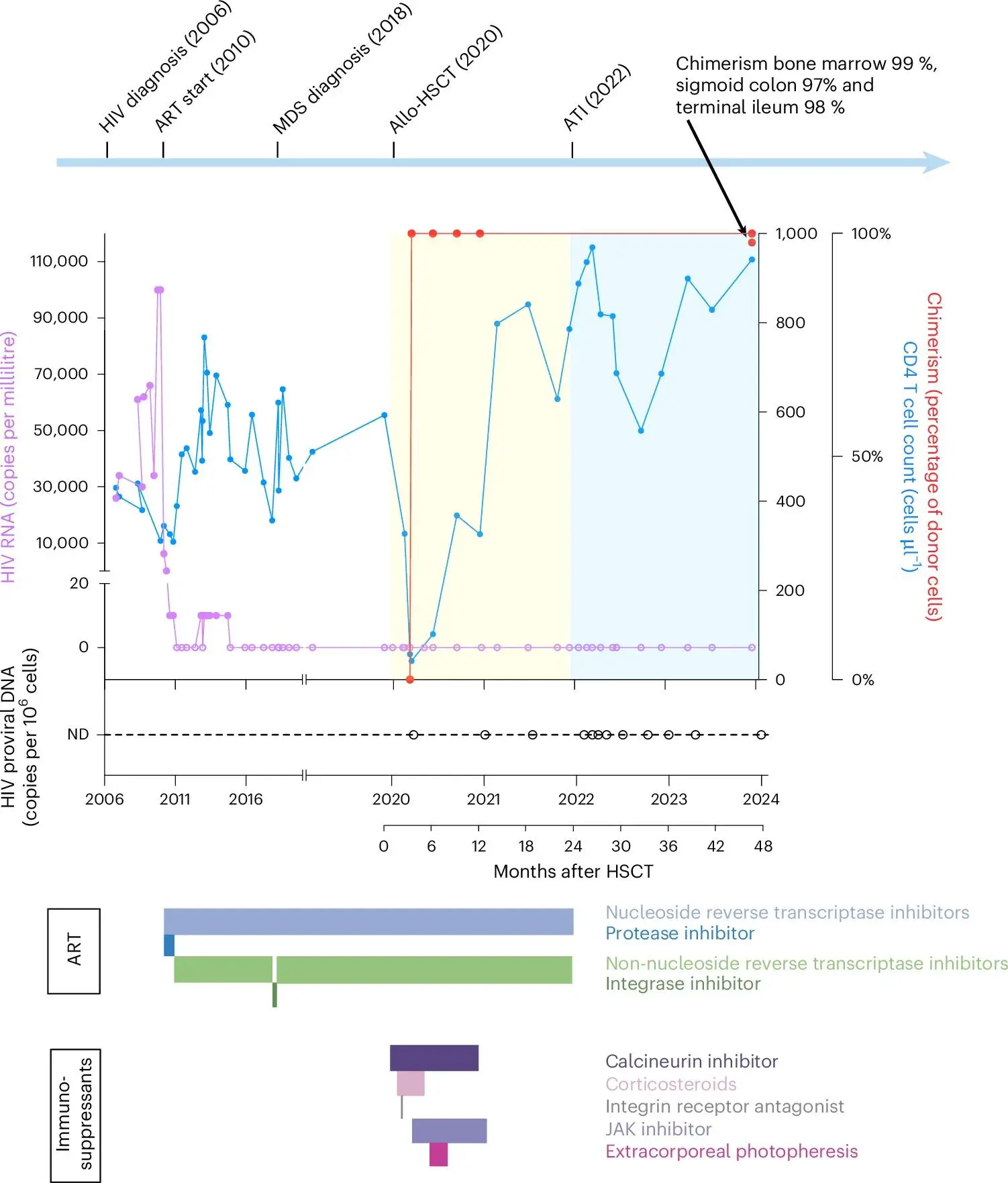
As reported by Nature, the man was given a bone marrow stem cell transplant to treat his blood cancer. After researchers from Oslo University Hospital discovered the brother had the CCR5Δ32/Δ32 mutation, they monitored the situation to see if it had any effect on the virus.
Two years after the allogeneic (donor) hematopoietic stem cell transplantation (HSCT), the recipient was able to stop his HIV medication, and after five years, all traces of functioning HIV DNA have been eradicated.
Analyzing over 65 million immune system cells from the Oslo patient, there were no signs of the virus being able to replicate and no detectable HIV‑specific T-cell responses.
Cheering this breakthrough, researchers said: "The case of the Oslo patient contributes valuable evidence to the existing knowledge base regarding HIV cure cases.
"Moreover, this and other studies on HIV cure enhance our understanding of HIV pathology, molecular mechanisms, and predictive biomarkers that may be of broader interest, extending beyond patients treated with allogeneic HSCT."
Unfortunately, bone marrow stem cell transplants aren't viable for full HIV care because they're a risky operation and leave patients especially vulnerable to infections as they reboot the immune system.
More than this, it's unlikely that this scenario can be replicated in others. Siblings have around a 25% of being a transplant match, while the frequency of CCR5Δ32/Δ32 is only about % in northern European populations.
Researchers also noted that between 10 and 20% of those who receive stem cell transplants die within a year.
There are further complications, and in terms of the Oslo patient, he might've been effectively cured of HIV, but he also experienced a severe reaction that resulted in graft-versus-host disease.
Still, the immune system reaction and the drugs used to combat the graft-versus-host disease might have been partially responsible for ridding the Oslo patient of his HIV.
Looking at next steps, researchers concluded: "Moving forward, a critical step will be to compare existing cases of HIV cure to identify the most effective combination of biomarkers.
"Conducting individual patient data meta-analyses is a logical next step, ideally followed by prospective sampling and new analyses that apply harmonized protocols in centralized laboratories."
As research carries on, there's no escaping the fact that the Oslo patient is now only the tenth person who's reportedly been cured of HIV.